Aug. 18, 2023 – Elizabeth Svoboda was just 15 years old when she developed bouts of gnawing pain in her lower belly so bad, she would have to lie in the fetal position for hours until it subsided. Every few weeks, and for the next 2 decades, the sensation would return, disabling her.
“I’ve been through labor, and I would say that at its worst, my pain was comparable to that,” said Svoboda, now 42, of California.
It wasn’t until college that she addressed her pain with a doctor who, without doing any tests or imaging, ultimately chalked it up to irritable bowel syndrome (IBS): an intestinal disorder known for causing belly pain, gas, diarrhea, and constipation.
“At that point, I sort of threw up my hands and said to myself, ‘Nobody is going to be able to figure this out,’” Svoboda said. “I just accepted that this was my normal state of being.”
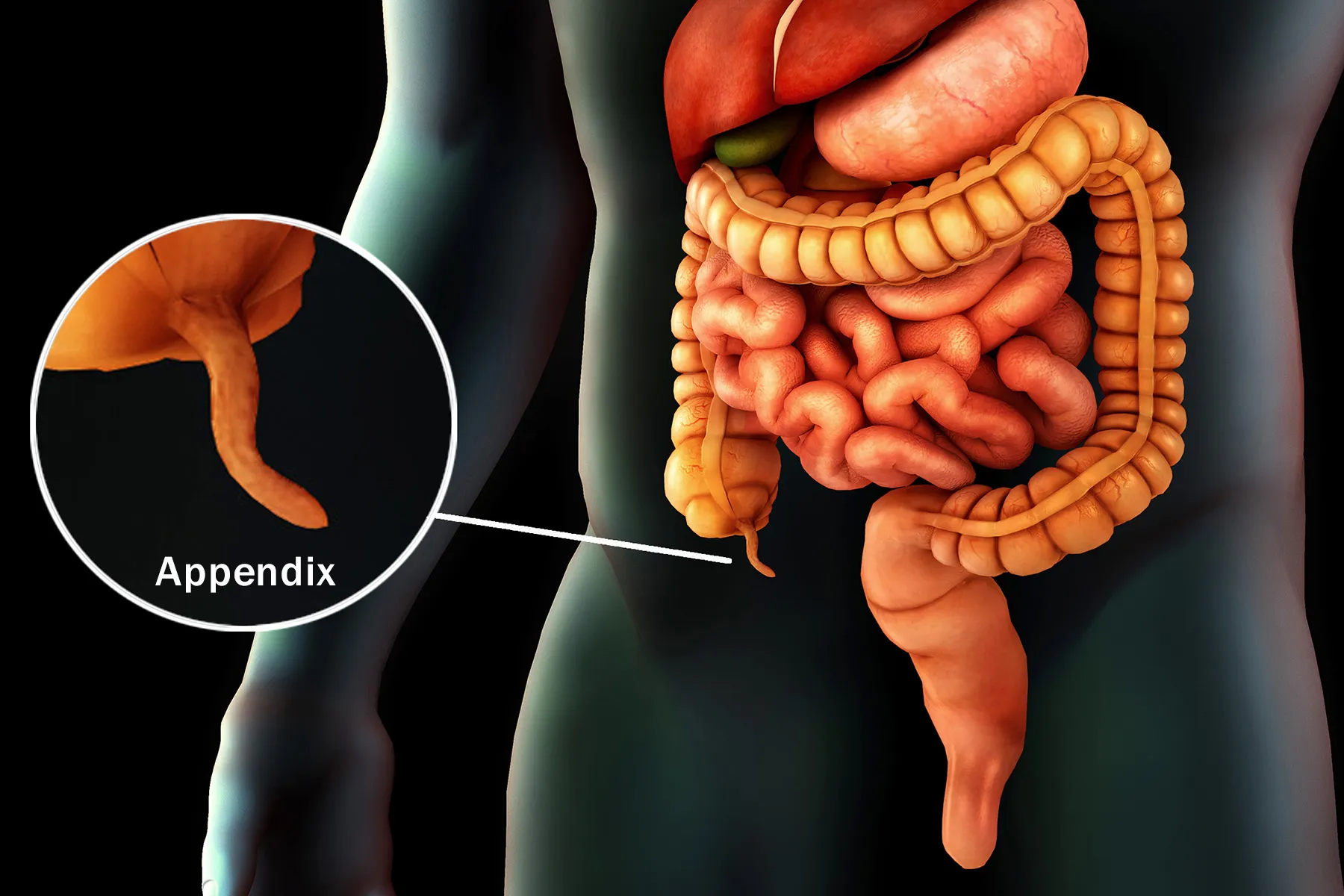
Little did she know, it would take nearly 20 years of pain to figure out what plagued her: chronic appendicitis. Although no official definition exists, a person is thought to have the condition when their appendix, that finger-like pouch at the end of your colon, becomes inflamed and causes belly pain in regular on-and-off episodes that can span weeks, months, or years.
Chronic appendicitis is rare, according to current estimates. Studies have found that it occurs in about 1% of all cases of appendicitis, and affects adults and children alike.
Appendicitis is almost always acute, meaning it strikes suddenly and worsens quickly, sending people into emergency surgery to remove the organ. It occurs in 7% of the U.S. population, with 250,000 cases reported annually; most are diagnosed in people between 10 and 30 years old, but anyone can have it.
Both chronic and acute versions of the condition cause similar symptoms: pain that begins around the bellybutton and eventually moves to the lower right side of the belly, as well as nausea, vomiting, fever, and loss of appetite.
The main difference between the two is timing, said Reezwana Chowdhury, MD, a gastroenterologist and assistant professor of medicine at Johns Hopkins Medicine in Baltimore. Acute appendicitis typically comes on within 24 to 48 hours, while chronic appendicitis can come in episodes that last several hours and reappear randomly for at least a week, but usually more.
Because people with chronic appendicitis have pain that comes and goes, and typically isn’t severe enough to warrant a trip to the hospital, it can often be misdiagnosed as many other conditions, Chowdhury said, including but not limited to IBS, gastroenteritis, Crohn’s disease, or an infectious disease. CT scans and white blood cell counts, which are often elevated in those with acute appendicitis, can also come back normal, making chronic cases even harder to spot.
Experts don’t know what causes chronic appendicitis, but similar to acute cases, it’s believed to occur once the appendix becomes partially or completely blocked by hardened balls of stool, inflammation due to infection or other diseases of the gut, or cancerous growths, said Cherisse Berry, MD, chief of the Division of Acute Care Surgery at NYU Langone Health in New York City.
Appendicitis happens randomly, she said, so there aren’t definitive risk factors that might make one person more likely to have it over another.
These unknowns, researchers say, make it hard to know whether chronic appendicitis is the result of untreated acute appendicitis or if it’s a different disease altogether.
As scarce as cases may be, chronic appendicitis has been gaining traction in the medical community as a growing number of case reports on the condition are published in scientific journals. The first one was reported in 1949.
Still, the condition is considered a controversial diagnosis; many doctors have yet to treat a case themselves, and some aren’t aware it’s a real medical phenomenon.
“I have never seen a case of chronic appendicitis, and unfortunately I don’t know how often it’s in our differential for many patients that we see,” Chowdhury said. “The issue is that there’s no official diagnostic criteria, and it’s usually a diagnosis of exclusion,” meaning doctors diagnose the condition through the process of elimination.
Svoboda never actually received an official diagnosis. After unbearable pain landed her in the hospital right before Christmas 2012, a CT scan revealed she had acute appendicitis, and she had her appendix removed right away. It was only after extensive research and chats with her father, who’s a doctor, that Svoboda realized her condition was most likely the chronic kind.
“If I had a doctor that had known to look for chronic appendicitis, they might have been able to find it earlier and certainly change the course of my life for those more than 15 years that I had this pain,” said Svoboda, who says she’s been pain-free since her surgery. “That’s why I feel so strongly about raising awareness on this topic. If it could save people years of the kind of pain that I had, I think that would be a huge success.”
Prolonged Misdiagnoses Have Consequences
Chronic appendicitis isn’t considered an emergency, but it can turn into one the longer it goes undiagnosed or misdiagnosed.
An untreated appendix can eventually burst. The longer you wait to surgically remove the organ, the greater your chances of getting swelling in the lining of your belly called peritonitis or a pocket of pus called an abscess that could spread infection in the body.
More rarely, appendicitis can mask cancer of the appendix, which is why most doctors recommend patients have surgery instead of opting for antibiotic treatment, Berry said. CT scans won’t always catch cancers in the appendix, especially if they’re low-grade; in many cases, they can only be detected via lab work done on the appendix after it’s removed.
Appendiceal cancer is thought to affect one to two people per 1 million each year, according to the National Cancer Institute, but studies show it’s becoming more common, especially in people younger than 50.
Otherwise, the consequence of a late or incorrect diagnosis is weeks, months, or years of unnecessary pain. The good news: Studies have found that surgical removal of the appendix offers relief for most people with a chronic case.
Steven Teleky can attest to that. The 28-year-old San Francisco Bay Area resident started feeling stabbing pains around his bellybutton while at a baseball game in April. They eventually disappeared, so he thought lack of sleep was to blame. The next month, Teleky went to Portugal for a family vacation, and the intense pains came back.
“With every right step, boom, horrible shooting pain in my bellybutton,” he said. “Again, I chalked it up to anxiety of being in a new place, or heck, maybe even a hernia, and ignored it.”
A month after returning home, the pain came back in his lower right belly, this time causing extreme swelling in his pelvic area, as well as daily nausea that stripped his appetite.
Last week Teleky went to the hospital. Although he didn’t have severe pain at the time, the physician assistant in charge of his care was adamant about getting Teleky a CT scan, which found moderate inflammation in his appendix. He was quickly diagnosed with appendicitis and successfully had his appendix removed.
In a follow-up appointment, his surgeon confirmed he was dealing with chronic appendicitis, and he is now on the road to recovery.
“I’m very thankful that even though I was in the ER with no real pain, the physician assistant that saw me pushed for scans. Without her insisting on ruling out the worst-case scenario, who knows what would have happened,” Teleky said. “She really saved me a ton of headache — and likely saved my life.”
https://img.wbmdstatic.com/vim/live/webmd/consumer_assets/site_images/articles/health_tools/stomach_ache_what_could_it_be_slideshow/1800ss_science_source_rm_appendix_illustration.jpg
2023-08-18 19:51:28